Pelvic Floor Therapy
What is the Pelvic Floor?
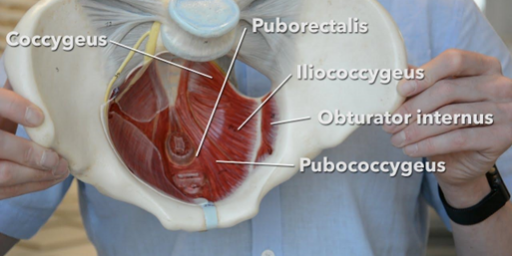
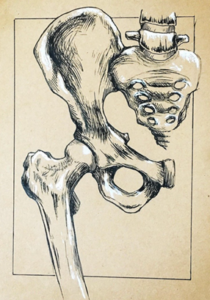
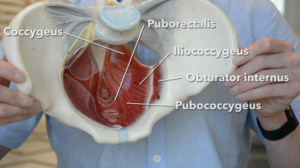
The pelvic region consists of several bones, ligaments, and muscles that essentially hold the abdominal organs, bladder, uterus, and bowels. The bony pelvis is made up of the sacrum (where your tailbone extends from), ileum, ischium, and pubis. The muscles that attach from the front of the pubis to the tailbone at the back are essentially the “floor” of the pelvis. Have a look at the diagram below for better visualization of the pelvic floor muscles. More than that, the function of the pelvic floor also works with abdominal and back muscles to help stabilize your core and spine.
What Are the Two Types of Pelvic Floor Muscles?
The pelvic floor is comprised of two types of muscles: the superficial and deep pelvic floor groups. The superficial muscles, such as the bulbospongiosus and ischiocavernosus, control urination, defecation, and support the genitals. The deep muscles, including the pubococcygeus and iliococcygeus, provide structural support for the pelvic organs and help regulate bowel movements. Both sets of muscles play a crucial role in maintaining urinary and bowel continence, sexual function, core engagement, and overall pelvic stability, making their health and coordination vital for overall well-being.
What is Pelvic Floor Dysfunction?
Dysfunction can occur for many reasons. Injuries to the pelvic region, surgeries, childbirth, chronic constipation, psychosocial factors like depression and anxiety, or even your occupation can contribute to changes in the pelvic floor.1,2 An important topic that is not often discussed and can be a major contributor to pelvic floor dysfunction is trauma. Trauma is a loaded word encompassing a single or ongoing emotional, mental, and/or physical event that can disrupt a person’s well-being.3 Often times I work with patients whose act of safety from trauma is to disconnect from the body, including the pelvic region, which can lead to pelvic floor dysfunction.
What Are the Symptoms of Pelvic Floor Dysfunction?
When dysfunction persists, it can lead to many different symptoms, including the following:
- Chronic pain
- Urinary incontinence
- Fecal incontinence
- Pelvic organ prolapse
- Sexual dysfunction
*Please note that this is not an exhaustive list.
What are the Benefits of Pelvic Floor Therapy?
All people can benefit from pelvic floor therapy, especially when suffering from the symptoms listed above. Pelvic floor therapy can promote relaxation, support and strengthen the muscles of the pelvis, decrease pain, improve bladder control, and promote healthy sexual function over time and with work. Additionally, patients can experience a deeper connection to their body. I have found that with this therapy, a space opens for patients to work through difficult emotions they are experiencing and have experienced in the past. Overall, patients may experience more ease physically, mentally, and emotionally.
Therapy for the Pelvic Floor
There are many ways to treat the pelvic floor, and many different providers to help you. Standard providers here in Oregon include physical therapists, physicians with extra training in pelvic floor therapy (that’s me!), and massage therapists, just to name a few. These providers will approach therapy differently but almost always use some form of manual therapy (physical touch) during their appointments. The shared goal is to restore and maintain function and movement in the pelvic floor and surrounding areas.
Speaking of my training, I address pelvic floor dysfunction with a “whole person” approach. This means that as I treat the physical body, I also consider the mental and emotional aspects. As mentioned earlier, there are many reasons for pelvic floor dysfunction, which means it requires a treatment approach that can address multiple areas.
What Exercises Does a Pelvic Floor Therapist Do?
Pelvic floor therapists employ a variety of exercises to address pelvic floor dysfunction. These exercises are prescribed based on whether your pelvic floor is too tight, too weak, or the muscle coordination is off. These may include Kegels, which involve contracting and relaxing specific pelvic muscles, but Kegels are not appropriate for every case. Therapists frequently use biofeedback techniques to help patients identify and control their pelvic muscles. Therapeutic exercises focus on strengthening and stretching the pelvic floor muscles as well as improving coordination and endurance. Overall, the goal is to alleviate issues like incontinence or pelvic pain, helping individuals regain optimal pelvic health and function.
What to Expect in Your First Pelvic Floor Therapy Visit
A first visit with me always includes a thorough intake. This allows me to review your history, discuss a possible diagnosis with you, and determine if other labs or imaging may be needed before moving forward with treatment. A first visit may also include a physical evaluation, but I typically converse with you first to determine your comfort level. Building trust and comfort is my priority.
How Many Appointments Will I Need?
Follow-up visits typically include manual therapy where I address the abdomen, lower back, pelvic region, and hips. Often times this can look like trigger point release, deep tissue massage, manual adjustments of the back and hips, and internal pelvic floor therapy. Depending on the goals of each patient, I may discuss exercises, as well as dietary and lifestyle modifications to further support you outside of the treatment room. Being a naturopathic doctor, I might also utilize herbs and homeopathic remedies for additional support for your mental and emotional well-being. (See my upcoming blog on my favorite herbs for the pelvic floor.)
On average, I aim for 4-6 sessions to get a solid idea of the problem and how to approach it, while giving you time to try new things and make changes. We will come up with a plan on how many visits to schedule to address your specific concerns. The amount of sessions can vary from person to person so I don’t have a hard rule on the number of treatments. Mostly, I want to make sure that the work we are doing is benefiting you so I will frequently check in to determine if it’s time for a different approach to your care.
How Quickly Can You Improve Pelvic Floor Dysfunction?
The speed at which you can improve your pelvic floor health depends on various factors, including the severity of the issue, your commitment to exercise, and the type of dysfunction you are experiencing. Some individuals may experience improvement in a few weeks with regular pelvic floor exercises, while others may take several months to see significant progress. Consistency and correct technique are essential. For a customized plan and direction to get the best outcomes in enhancing pelvic floor function, speak with a medical practitioner or pelvic floor therapist.
Conclusion
Perhaps you are experiencing symptoms talked about in this article, or maybe you are seeking to improve your connection to your body and pelvic floor. There are many benefits of this therapy and various ways it can be performed by different practitioners. Due to the sensitive nature of this therapy, I strongly recommend finding a practitioner that you trust and will hold a safe space for you. If you are unsure that pelvic floor therapy is the right treatment modality for you, a consult is the way to go! Let’s connect and see if we are the right fit.
Resources
- Bo K, Berghmans B, Morkved S, Van Kampen, M. Evidence-based Physical Therapy for the Pelvic Floor Bridging Science and Clinical Practice. 2nd edition. Elsevier Churchill Livingstone; 2015.
- Ghaderi F, Bastani P, Hajebrahimi S, Jafarabadi MA, Berghmans B. Pelvic floor rehabilitation in the treatment of women with dyspareunia: a randomized controlled clinical trial. Int Urogynecol J. 2019;30(11):1849-1855. doi:10.1007/s00192-019-04019-3
- Trauma and violence. SAMHSA. September 27, 2022. Accessed October 3, 2023.
https://www.samhsa.gov/trauma-violence - Webster, S PhD. Pelvic Floor Anatomy.
https://youtu.be/D4Mrytn9Cw0?si=sqD5ajjlK5URIuOT. Published May 31 2017. Accessed October 3 2023.